Most U.S. dental practices lose between 5% and 12% of collectible revenue every year, not because of clinical production shortfalls, but because of small, preventable errors in their billing process. On average, dental practices lose about 9% of collectible revenue annually due to missed billing processes, and the culprits hide in both insurance billing and patient billing workflows.
At Prospa Billing, we audit hundreds of practices’ revenue cycle operations and consistently find the same patterns: preventable write-offs from unworked denials, bad debt from inconsistent patient collections, and slow cash flow caused by broken handoffs between verification, claim submission, and follow up.
Dental insurance billing is the process of creating, submitting, following up, and collecting payment from insurance claims; a process complicated by factors like patients’ insurance changes and annual code updates. Patient billing, in contrast, focuses on calculating and collecting the patient’s portion: copays, deductibles, coinsurance, and balances left after insurance adjudication.
This article compares where money leaks from each billing stream and how to plug those leaks. You’ll see concrete examples, like verification failures that cause denials, unnecessary adjustments that mask underpayments, and lack of follow up that turns valid claims into write-offs, along with practical fixes for your dental practice.
How the Dental Revenue Cycle Really Works (and Where Cash Gets Stuck)
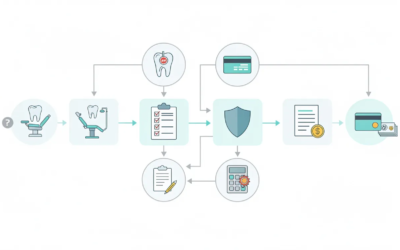
The revenue cycle in a dental practice isn’t a single pipeline. It’s two intertwined streams that flows smoothly to protect your financial health. Here’s how the full cycle breaks down:
- Scheduling and registration: New patients provide insurance information and demographics
- Verification and pre-authorization: Confirming active insurance coverage, benefits, waiting periods, and exclusions before the appointment
- Treatment planning: Documenting procedures performed and creating accurate patient estimates
- Clinical documentation: Capturing clinical notes, periodontal charting, radiographs, and supporting documentation
- Claim submission: Sending electronic claims to payers via clearinghouses with correct CDT codes and attachments
- Payment posting: Reconciling Explanation of Benefits documents line-by-line against your fee schedule
- Patient billing: Calculating residual balances and collecting payment from patients
- Follow up: Working denials, aging insurance A/R, and patient collections systematically
Even small delays compound into serious cash flow issues. A 45-day insurance claim instead of a 15-day claim might seem minor, but multiply that delay across hundreds of claims and you’ve created a substantial bottleneck. Outsourced revenue cycle management focuses on tightening each handoff, not just pushing out more claims.

Top Leak Points That Quietly Kill Reimbursement in Dental Insurance Billing
Insurance billing is the most complex part of the dental billing process and the biggest source of hidden write-offs. Approximately 65% of dental practices participate with dental insurance, making dental billing a crucial component in a practice’s revenue cycle management.
Most insurance revenue loss occurs before the claim is even created: at eligibility verification, benefit breakdowns, and coding decisions. Prospa Billing typically finds 3-8% of annual production lost to preventable insurance write-offs, missed filing limits, and unworked denials. Common issues in dental insurance billing often come from simple administrative errors, outdated information, or missing documentation.
While practice management software and technology help, consistent processes and trained dental billers are what actually protect cash flow by reducing common dental claim denials that slow reimbursement. Let’s break down the specific leak points.
Leak #1: Weak Insurance Verification and Benefit Breakdown
Insurance verification involves confirming coverage, active benefits, and any waiting periods or exclusions before the appointment. When this step fails, denials follow.
Common verification gaps include:
- Not confirming active coverage on the exact date of service
- Missing plan frequency limits (e.g., one crown per 5 years)
- Overlooking waiting periods for major restorative work
- Failing to check coordination of benefits with secondary payers
- Not documenting deductible status or remaining annual maximums
Example: A crown performed on 02/15/2026 gets denied because the patient’s primary insurance plan terminated on 01/31/2026. The treating dentist never verified COB, and now the practice faces full patient responsibility or write-off.
Implementing real-time verification of active coverage and deductible limits can help avoid many billing issues. A standardized verification checklist documented in your practice software prevents these denials and protects both practice and patient from surprise out of pocket costs.
Leak #2: Incomplete Clinical Documentation and Incorrect Coding
Accurate and complete documentation is essential to avoid denied claims, reduced reimbursement, and compliance issues. Small errors in coding or documentation can lead to significant delays in payment.
Typical documentation gaps:
- Missing periodontal charting for scaling and root planing claims
- Absent radiographs or intraoral images
- No narrative justifying medical necessity for crowns
- Failure to document failed prior restorations
Coding issues that trigger problems:
- Using incorrect CDT codes or diagnosis codes
- Not coding multiple surfaces correctly (e.g., D2391 for mesial-occlusal)
- Ignoring annual Current Dental Terminology updates from the American Dental Association
- Miscoding limited (D0145) versus comprehensive exams (D0150)
Missing documentation, such as X-rays and clinical notes, is often necessary to establish medical necessity for claims. These errors trigger denials, medical review, or downgraded payments, increasing accounts receivable days and staff time on rework. Prospa Billing trains billers to cross-reference clinical notes with accurate codes and request missing documentation before claim submission—not after a denial.
Leak #3: Sloppy Claim Submission and Missed Filing Limits
Claims processing delays often stem from preventable submission errors. Many practices still batch claims weekly instead of submitting claims promptly within 1-2 business days post-treatment.
Common submission errors:
- Wrong subscriber ID or misspelled patient names
- Missing tooth numbers or procedure locations
- Incorrect rendering provider NPI
- Outdated payer IDs or clearinghouse addresses
- Inaccurate patient information such as incorrect dates of birth—a leading cause of claim rejections
Timely filing limits are critical, as claims submitted late may be automatically rejected by insurers. Many PPOs enforce strict 90-day requirements, turning valid claims into pure write-offs. Most clean dental claims are typically paid within 14 to 30 days, but longer timelines indicate issues like missing documentation requirements or payer-specific insurance rules.
Daily electronic claim submission with built-in validation rules keeps your insurance cash cycle under 20-30 days and dramatically reduces these leak points, especially when supported by specialized dental insurance billing services that manage submissions and follow up consistently.
Leak #4: Inaccurate Payment Posting and Over-Generous Adjustments
Payment posting quality directly impacts accurate write-offs and performance reporting. An Explanation of Benefits is provided after processing a claim, summarizing charges, payments made by insurance, and any remaining balance owed by the patient.
Key risks:
- Posting payments at the claim level instead of line-item level, hiding chronic underpayments
- Using generic “insurance adjustment” or “PPO write-off” codes to force-balance accounts
- Not reconciling EOBs against current fee schedules
Example: A $1,200 implant-supported crown gets posted with a $300 unexplained adjustment because staff didn’t compare the EOB to contracted rates. That $300 disappears as an unquestioned write-off.
Prospa Billing uses standardized adjustment codes, reconciles each EOB to contract terms, and flags chronic underpayments for follow up or renegotiation with the insurance company, mirroring the end-to-end focus described in how dental billing works and where practices lose money.
Leak #5: Inconsistent Follow Up on Insurance A/R and Denials
Unworked insurance A/R over 60 days is often the single largest bucket of hidden cash in a dental practice. Regularly reviewing insurance accounts receivable, ideally on a weekly basis, helps practices address issues early and prevent revenue loss due to denied claims—exactly the kind of day-to-day work a dental insurance billing company handles for outsourced clients.
Common failures:
- No weekly aging reports generated or reviewed
- No clear owner assigned to work aging insurance balances
- No aging-based work queues for staff
- Ignoring payer-specific follow-up protocols
Example: A practice with $250,000 in unpaid insurance A/R discovers that 45% exceeds 90 days—much of it still appealable but untouched due to lack of process.
Filing detailed appeals promptly after a claim denial, along with reviewing the EOB for specific reasons, is important for resolving denied claims. Prospa Billing assigns dedicated teams to work denials and aging buckets systematically, recovering revenue that would otherwise become bad debt.

Where Bad Debt and Patient Friction Erode Profit in Patient Billing
While patient balances are usually smaller per visit than insurance amounts, they accumulate into significant bad debt when processes are weak. Dental practices can lose up to 9% of collectible revenue annually due to missed billing processes, which directly impacts cash flow management.
Patient billing distinguishes between responsibility at time of service (copays, deductibles, coinsurance) and residual balances after insurance payment posting. Many practices focus heavily on insurance billing but leave patient billing to sporadic statements and uncomfortable front-desk conversations.
Main leak areas include inaccurate estimates, lack of financial agreements, slow statements, and inconsistent collections policies. Outsourced patient billing and statements services can help standardize communication and reminders so a confusing billing experience doesn’t undo excellent patient care and drive new patients away, damaging patient satisfaction and financial stability.
Patient Leak #1: Inaccurate Treatment Estimates and No Upfront Financial Agreement
“We’ll bill you later” is a major revenue risk. Not using real-time insurance benefits information leads to under-estimating patient responsibility, creating surprise balances after EOBs arrive.
Example: A $3,000 treatment plan in March 2026 where the practice collects only $500 based on a rough guess. When the insurance claim processes, a $900 surprise balance emerges. Without a signed financial agreement, the patient disputes the charge, and it ages into write-off.
Clear financial policies, accurate estimates using verified benefits, and signed agreements that spell out payment expectations drastically reduce disputes and bad debt. Financial assistance options and payment plan discussions should happen before dental procedures, not after.
Patient Leak #2: Weak Point-of-Service Collections
Collecting payment at the time of service is critical for maintaining cash flow.
Common issues:
- Staff uncomfortable asking for payment or lacking scripts
- No card-on-file system for future payments authorization
- No same-day payment options or structured approach
- Collecting “whatever they can pay today” without process
Effective tactics for collecting payment:
- Card-on-file authorization at registration
- Payment plans through integrated software or CareCredit financing
- Training staff with clear scripts for discussing copays and deductibles
- Targeting 90%+ collection of estimated patient responsibility same-day
Prospa Billing encourages practices to collect patient responsibility on or before the day of service. Healthcare services delivered without clear payment expectations create chronic aging patient A/R.
Patient Leak #3: Slow, Confusing Statements and Limited Payment Options
Even with strong point-of-service collections, post-visit billing still matters. Efficient billing processes are crucial for maintaining consistent cash flow, as delays in payment lead to financial strain.
Problems to avoid:
- Sending statements only once a month
- Unclear line items that don’t specify services rendered
- No email, text, or bill online options
- No digital payment portal
Each extra week between service, insurance posting, and first statement reduces the patient’s motivation to pay. Practices should send clear, itemized statements within 7-10 days after insurance payment posting, with multiple digital payment options. Integrating billing systems with payment portals automates this process and shortens time to receive payment.
Patient Leak #4: Inconsistent Collections Policies and Overuse of Write-Offs
Many practices oscillate between being too lenient and too aggressive with patient collections.
Common issues:
- No standardized timeline for reminders
- Unclear criteria for sending accounts to collections
- Ad-hoc “courtesy” write-offs to avoid uncomfortable conversations
- No documentation of collection attempts
A structured ladder of communication works:
- Day 10: Friendly email reminder
- Day 30: Text message and phone call
- Day 60: Payment plan offer
- Day 90: Clear steps toward external collections or final write-off
Repeated small courtesy discounts accumulate into thousands of dollars annually. Prospa Billing helps define these policies, track patient A/R aging, and report on where write-offs originate.
Insurance Billing vs Patient Billing: Revenue Risk and Control
Both billing streams share core process steps—verification, claim or statement creation, payment posting, and follow up—but differ in rules, timelines, and emotional dynamics, and a unified approach to streamlining insurance and patient payments ensures neither side quietly erodes profitability.
| Aspect | Insurance Billing | Patient Billing |
|---|---|---|
| Primary risk | Denials, underpayments, write-offs | Non-payment, bad debt |
| Timeline pressure | Strict filing limits (90-180 days) | Flexible but aging reduces collection |
| Control level | Limited—payer rules dictate much | Higher—policies and communication matter |
| Resolution approach | Appeals, resubmissions, documentation | Empathy, reminders, payment options |
Many practices overestimate their control over insurance and underestimate how much control they have over patient billing through clear communication and policies. The strongest practices build clean, documented workflows for each stream separately.
Which Side Loses You More Money Today?
Two diagnostic questions help identify your bigger leak:
- What percentage of production is written off due to insurance issues? (Target: under 5%)
- What percentage of patient receivables roll past 90 days? (Target: under 10%)
Regularly reviewing accounts receivable, especially balances aging beyond 30 and 60 days, is essential for identifying issues early and preventing revenue loss. Proper management of the insurance aging report, which lists outstanding claims, is crucial for maintaining healthy cash flow.
Prospa Billing uses audits of these metrics during onboarding to identify whether a practice’s bigger opportunity lies in insurance billing optimization or patient billing cleanup, then recommends the right mix of dental billing services for growing practices. Quantify your leak instead of guessing—that’s the first step to protecting cash flow.
Designing a Clean Insurance Billing Process That Protects Every Claim
A clean insurance billing process is a series of checklists and standard operating procedures—not just experienced people. The goal: reduce denials, speed up medical claims and dental insurance claim payments, and minimize unnecessary write-offs through consistent steps followed every time.
Implementing AI-powered tools can assist with key billing functions, helping to reduce denials, shorten the time to payment, and stabilize cash flow by flagging potential claim issues before submission. An efficient dental billing process involves clear procedures, expert support, and automation, whether you manage it in-house or use outsourced dental billing to balance cost, control, and risk.
Real impact: practices that systematize these workflows often cut insurance A/R over 90 days in half within six months.
Core Elements of a High-Performing Insurance Billing Workflow
- Daily verification: Check eligibility and insurance benefits for all scheduled patients; document notes in practice management software
- Same-day submission: Create and submit claims electronically on the same day as procedure posting with attachments and narratives
- Line-item posting: Post payments against EOBs at the line level; flag discrepancies and categorize denial codes
- Structured follow up cadence:
- 20 days: Check claim status
- 30 days: Escalate unresolved claims
- 60+ days: Prioritize for appeals or resubmission
Dental medical billing allows dentists to receive medical insurance reimbursements for medically necessary procedures, expanding patient access to health care services and diversifying practice revenue. Unlike dental insurance, medical billing requires precise coding, thorough documentation, and strategic claim submission.
Designing a Clean Patient Billing Process That Reduces Bad Debt
Patient billing needs its own clearly defined process—not leftover attention after insurance work finishes. The objective: collect as close to 100% of patient responsibility as possible while maintaining positive patient experiences.
Clear policies, modern payment options, and empathetic communication reduce friction and bad debt. Prospa Billing helps practices align patient billing with insurance workflows so balances are identified and pursued immediately after payment posting.
Core Elements of a High-Performing Patient Billing Workflow
- Pre-treatment financial consultations: Use verified insurance data to present printed or digital estimates; discuss services covered and pocket costs upfront
- Day-of collection: Collect deposits or full estimated patient responsibility with saved cards, financing options, or payment plans
- Rapid residual statements: Generate and communicate balances within 7-10 days of insurance payment posting—not at month-end
- Consistent reminder sequence: Email, text, and phone over 60-90 days before considering accounts for collections or internal write-off
The dental medical billing process involves patient registration, insurance verification, procedure coding, claim submission, payment posting, and follow-up on claims. This applies to both medical services and dental services when medically necessary.

How Prospa Billing Helps Practices Plug Both Insurance and Patient Revenue Leaks
Prospa Billing is a specialized dental revenue cycle management partner focused on insurance billing, patient billing, and collections. We integrate with common dental practice management systems to handle claim submission, payment posting, denial follow up, and patient statement workflows.
Our teams are trained specifically in dental coding, insurance requirements, and patient billing best practices, not generic medical billing alone. We understand out of network provider challenges, payer-specific documentation requirements, and the nuances of health plans that affect reimbursement.
Tangible outcomes practices can expect:
- Reduced insurance A/R aging (often from 60+ days to under 30)
- Fewer write-offs through systematic denial appeals
- Faster cash flow through daily claims processing
- Lower patient bad debt via structured collections
Contact customer service to request a billing process audit or consultation. We’ll identify your top insurance and patient billing leak points and build a step-by-step plan to address them.
Build Parallel, Clean Processes to Protect Every Dollar You Earn
Most lost revenue in dental practices stems from process gaps in insurance billing and patient billing, not lack of production. Dental billing is the process of submitting and following up on claims for payment for dental services provided to patients, involving preparation of claims for insurance companies, government programs, or patients themselves.
Treat insurance billing and patient billing as distinct but coordinated workflows, each with its own verification, posting, and follow-up steps. Review at least one year of write-offs and A/R reports to quantify your leak and prioritize fixes. Knowledge of where your money disappears is the foundation for stopping the loss.
Connect with Prospa Billing for a tailored revenue cycle review and step-by-step plan to strengthen both sides of your billing process. Tighter processes create predictable cash flow, less stress for staff, and better experiences for patients—protecting your practice’s financial future one claim at a time.



0 Comments